A Step-by-Step Playbook for Digitizing Every Patient Touchpoint
How forward-thinking health systems are using healthcare-native AI to connect every clinical and operational workflow, from admission to discharge and beyond.
Introduction: Why Every Touchpoint Matters
Walk through any modern hospital and you will notice something paradoxical. The operating rooms house robots capable of sub-millimeter precision. The pharmacy uses automated dispensing cabinets that track every pill. Yet in the hallway between those two departments, a nurse is likely carrying a printed sheet of paper from one workstation to another, manually re-entering information that already exists somewhere else in the building.
This is the reality of healthcare in 2026. Pockets of extraordinary technology coexist with workflows that have barely changed in decades. Every manual handoff, every re-keyed data point, every unstructured note that never gets read is an opportunity for error, delay, or missed insight.
Digitizing every patient touchpoint is not about replacing clinicians with algorithms. It is about ensuring that every interaction, from the moment a patient schedules an appointment to the day they complete their post-discharge follow-up, generates data that is connected, structured, and actionable. When that foundation is in place, something remarkable happens: the hospital starts to learn from itself.
| The goal is not automation for its own sake. It is building a health system where information flows as naturally as the clinicians who depend on it. |
This playbook lays out a practical, step-by-step approach to achieving that vision. Each chapter addresses a layer of the digital hospital (data infrastructure, clinical reasoning, workflow automation, safety surveillance, and operational intelligence) with concrete guidance on what to implement and why it matters. The tools and capabilities described here are drawn from John Snow Labs’ healthcare AI ecosystem, which has been purpose-built for the clinical domain from the ground up.
Building the Data Foundation
Every ambitious digital health initiative that fails shares a common root cause: fragmented data. It does not matter how sophisticated your AI models are if the information feeding them is scattered across disconnected systems, trapped in incompatible formats, or buried in unstructured clinical notes that no machine has ever parsed.
Building a fully automated hospital begins, therefore, not with flashy AI capabilities but with the unglamorous, essential work of unifying your data assets. This means creating pipelines that bring together structured EHR fields, free-text clinical narratives, radiology and imaging metadata, and increasingly, genomic and pathology insights. All into a single, coherent data layer that supports real-time access and analytics.
The Integration Challenge
Most hospitals operate dozens of clinical and administrative systems that were never designed to talk to each other. The EHR captures one slice of reality. The radiology PACS captures another. Laboratory information systems, pharmacy dispensing platforms, and billing engines each maintain their own version of the patient’s story. What is missing is a unifying intelligence layer that can reconcile these sources and make them collectively useful.
John Snow Labs’ healthcare data pipelines address this challenge directly. Rather than requiring hospitals to rip and replace existing systems, these pipelines sit on top of your current infrastructure, ingesting data from multiple sources and harmonizing it into a common clinical data model. Structured fields are normalized. Unstructured text is parsed using clinical NLP. Coded data is mapped to standard terminologies. The result is a unified foundation that downstream applications can reliably consume.
Why Real-Time Matters
Batch processing was acceptable in an era when clinical decisions were made over days or weeks. Today, clinicians need information at the point of care in real time. A sepsis risk score computed overnight is clinically useless for the patient who deteriorated at 3 AM. An adverse drug interaction flagged after the medication has been administered is an incident report, not a prevention tool.
The data foundation described here is designed for streaming, low-latency access. As new data enters the system (a lab result, a nursing note, an imaging study) it is immediately available for reasoning and alerting. This is what transforms a hospital’s data infrastructure from a passive repository into an active participant in patient care.
Clinical Reasoning at Scale
For decades, clinical decision support meant rigid, rule-based alerts, the kind that interrupt clinicians with pop-ups they quickly learn to ignore. Static rules cannot account for the complexity, nuance, and ambiguity that define real clinical reasoning.
Medical large language models change the equation fundamentally. Instead of matching patterns against pre-defined rules, these models reason over clinical context in ways that mirror, and in some dimensions exceed, what a human expert can process. They read entire patient histories, weigh competing diagnoses, and synthesize evidence from multiple sources, all in seconds.
How the Medical Reasoning LLM Works
John Snow Labs’ Medical Reasoning LLM is not a general-purpose language model that has been superficially fine-tuned on medical text. It is a purpose-built system trained specifically for clinical reasoning, with architecture and training data designed around the way healthcare professionals actually think.
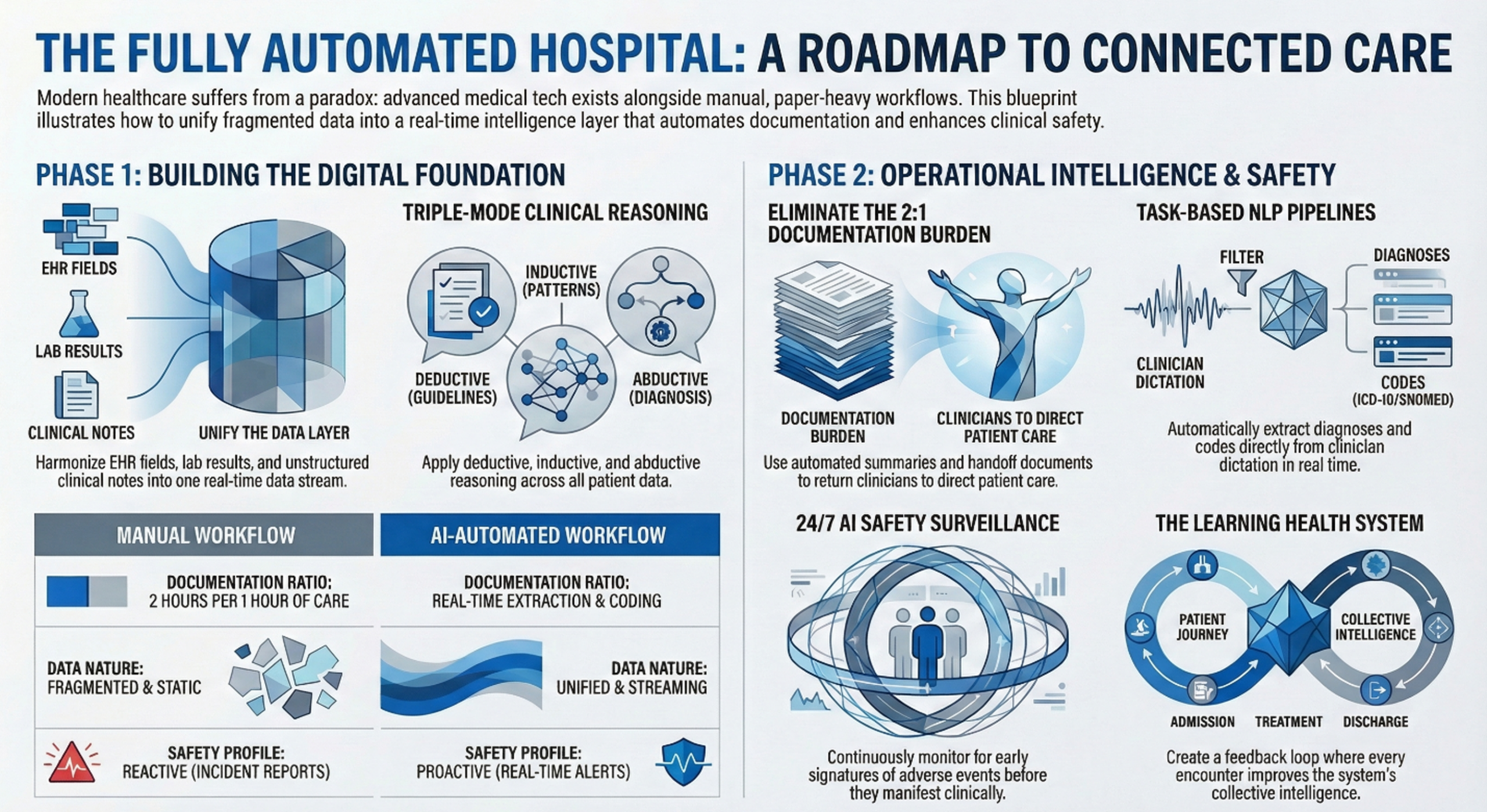
The model supports three fundamental modes of clinical reasoning. Deductive reasoning applies established guidelines and protocols to specific patient scenarios. If a patient presents with these symptoms and these lab values, then this clinical pathway applies. Inductive reasoning identifies emerging trends from patient data, recognizing patterns that might not yet be codified in clinical guidelines. Abductive reasoning generates the most likely explanations for a set of observations, which is precisely what clinicians do when they build a differential diagnosis.
| Clinical AI is not about replacing the physician’s judgment. It is about giving every clinician access to the reasoning depth and breadth that only the most experienced specialists currently possess. |
Automating the Documentation Burden
Ask any physician what they would change about their daily work and the answer is almost always the same: less time documenting, more time with patients. Studies consistently show that clinicians spend one to two hours on documentation for every hour of direct patient care. This is not merely an inconvenience but a primary driver of burnout, and burnout is a primary driver of medical error.
The documentation challenge is not that clinicians write too much. It is that so much of what they write must then be manually transformed, coded into billing classifications, extracted into quality metrics, reformatted for referral letters, summarized for handoffs. Each of these transformations is a repetitive, error-prone task that is ideally suited for automation.
Task-Based NLP Pipelines
John Snow Labs provides a suite of task-based NLP pipelines that operate on clinical text at the point of creation. When a physician dictates or types a clinical note, these pipelines can simultaneously extract key clinical entities (diagnoses, medications, procedures, lab values) and map them to standardized codes such as ICD-10 and SNOMED CT. What previously required a human coder reviewing the note hours or days later now happens in real time.
Beyond coding, these pipelines generate structured summaries of clinical notes, produce handoff documents for shift changes, and extract relevant information for referral letters. The clinician writes once, and the system handles the downstream transformations. This is not a marginal improvement; it is a fundamental restructuring of the documentation workflow.
Preserving Clinical Nuance
A common concern with automated documentation tools is the loss of nuance. Clinical language is rich with hedging, negation, and contextual modifiers. A note that says “the patient denies chest pain” means something entirely different from “the patient has chest pain.” Earlier NLP systems frequently stumbled on these distinctions, producing extraction errors that undermined clinical trust.
The NLP models from John Snow Labs are trained specifically on clinical text, with explicit handling of negation, speculation, family history references, and temporal modifiers. They understand that “no evidence of malignancy” is not a cancer diagnosis and that “mother had diabetes” is a family history finding, not a current condition. This clinical-grade precision is what separates healthcare-native NLP from generic text processing.
Validating AI with AI: The Evaluation Framework
Deploying AI in a clinical environment carries a responsibility that does not exist in most other industries. A recommendation engine that suggests the wrong movie wastes a few minutes of someone’s evening. A clinical AI that surfaces the wrong diagnosis can alter the course of a patient’s life. This is why rigorous evaluation is a prerequisite.
John Snow Labs approaches this challenge through what is known as the LLM-as-a-Judge framework, implemented within a dedicated medical LLM environment. It is an evaluation platform where clinicians and data scientists can systematically test, compare, and validate AI model outputs before those models are deployed in clinical settings.
How the Evaluation Framework Operates
The framework allows clinical teams to submit real-world queries (diagnostic questions, treatment planning scenarios, guideline interpretation tasks) to multiple medical LLMs simultaneously. The outputs are presented side by side, enabling direct comparison of reasoning quality, factual accuracy, and clinical appropriateness.
Crucially, the system goes beyond simple accuracy metrics. It evaluates whether models exhibit clinical bias, whether they handle edge cases and rare conditions appropriately, and whether their reasoning is transparent enough for a clinician to understand and verify. In a field where explainability is as important as accuracy, this depth of evaluation is essential.
Safety Surveillance and Compliance
Patient safety has traditionally been a reactive discipline. Something goes wrong, an incident report is filed, a root cause analysis is conducted, and a process change is implemented weeks or months after the event. This cycle has saved lives, but it is fundamentally limited by its dependence on human detection of adverse events, which studies suggest captures only a fraction of actual occurrences.
AI-powered surveillance changes this paradigm. By continuously reasoning over patient records, laboratory results, medication orders, and nursing documentation, surveillance models can detect the early signatures of adverse events before they fully manifest.
Real-Time Adverse Event Detection
John Snow Labs’ surveillance models monitor the full spectrum of clinical data streams for patterns associated with known adverse events. A subtle change in renal function following a medication adjustment, a rising inflammatory marker in a post-surgical patient, an unexpected shift in vital sign trends. All these signals are identified, correlated, and escalated in real time.
The system also monitors infection patterns across the institution, enabling early detection of outbreaks before they spread through clinical units. For quality assurance teams, every alert and escalation generates an audit-ready output, documenting what was detected, what evidence supported the alert, and what action was recommended. This continuous, automated surveillance creates a safety net that operates twenty-four hours a day, every day, something that no manual monitoring program can achieve.
Guideline Adherence Tracking
Compliance with clinical guidelines is another area where continuous monitoring outperforms periodic audits. Rather than reviewing a sample of charts every quarter, AI-powered compliance tracking evaluates every patient encounter against applicable guidelines in real time. Deviations are flagged immediately, allowing clinical teams to correct course while the patient is still under their care rather than discovering the gap during a retrospective review.
Toward Autonomous Health Systems
Everything described in the preceding chapters represents technology that is available and deployable today. But the trajectory of healthcare AI points toward something more ambitious: agentic systems capable of autonomous monitoring, reasoning, and action within defined clinical guardrails.
John Snow Labs’ Medical Reasoning LLM and Generative AI Lab already support the building blocks of this future. Task chaining allows multiple AI capabilities to be orchestrated into end-to-end decision workflows: a lab result triggers a risk calculation, which triggers a clinical alert, which populates a recommended order set. Autonomous clinical alerting systems monitor patient streams continuously and escalate concerns without waiting for a human to query the system. Real-time evidence synthesis pulls together information across modalities (text, imaging, laboratory data) to provide a comprehensive clinical picture.
Multimodal Intelligence and Precision Medicine
The next frontier involves multimodal AI models that reason simultaneously across imaging, genomics, and clinical text. Today, these data types are analyzed in silos: a radiologist reads the scan, a geneticist interprets the panel, a clinician synthesizes both reports. Multimodal models promise to integrate these analyses, enabling precision medicine at a scale and speed that siloed expertise cannot match.
The ultimate vision is the learning health system: an institution that continuously improves its own care delivery by learning from every patient encounter. Every diagnosis confirmed, every treatment outcome observed, every near-miss detected feeds back into the system’s intelligence, making it incrementally better at serving the next patient. This is not science fiction. The foundational components exist today. What remains is the work of integration, validation, and thoughtful deployment.
Conclusion: A Sequence of Integrated Steps
The fully automated hospital is not a destination you reach with a single technology purchase or a twelve-month implementation plan. It is a deliberate sequence of integrated steps, each building on the one before.
It begins with data: unifying the fragmented information sources that every hospital manages today into a coherent, real-time data layer. It continues with intelligence: deploying clinical reasoning models that can process patient histories with the depth and nuance of an experienced specialist. It extends into workflow automation, where NLP pipelines eliminate the repetitive documentation tasks that consume clinician time. It is reinforced by evaluation frameworks that ensure AI outputs meet clinical standards before they reach the bedside. And it is sustained by safety surveillance and operational optimization that make the hospital not just smarter, but safer and more efficient.
| The question for health system leaders is not whether to pursue this transformation, but how quickly they can begin and how thoughtfully they can execute it. |
John Snow Labs’ healthcare AI ecosystem provides the complete toolkit for this journey: data pipelines for integration, task-based NLP for documentation automation, the Medical Reasoning LLM for clinical intelligence, the LLM-as-a-Judge chatbot for rigorous evaluation, and the Generative AI Lab for building and chaining AI workflows without writing code. These are not experimental technologies. They are production-ready tools being used by health systems today.
The fully automated hospital is within reach. The playbook is clear. The only question that remains is: when do you start?
Frequently Asked Questions
How does John Snow Labs support EHR integration?
John Snow Labs’ healthcare data pipelines are designed to connect with existing EHR systems without requiring a rip-and-replace approach. The pipelines ingest both structured data (coded fields, lab values, medication lists) and unstructured data (clinical notes, discharge summaries, radiology reports), harmonizing them into a OMOP common data model that supports real-time access and AI-powered reasoning.
Can these tools be used by non-technical staff?
Yes. The Generative AI Lab is specifically designed for users who are not software developers. It provides a visual interface for chaining models, validating outputs, and building reasoning pipelines without writing code. This means that clinical informaticists, quality officers, and operational analysts can build and modify AI workflows directly, without depending on a dedicated engineering team for every change.
What about data privacy and regulatory compliance?
All tools in the John Snow Labs ecosystem support on-premise and private-cloud deployment, which means patient data never needs to leave the institution’s security perimeter. Role-based access control, comprehensive audit logging, and source citation for every AI output are built into the platform, supporting compliance with HIPAA, GDPR, and institutional governance requirements.
How should a hospital prioritize implementation?
Start with the data foundation. No AI initiative succeeds on fragmented data. Once your data pipelines are operational and your clinical information is unified, deploy task-based NLP for documentation automation. This delivers immediate, visible value to clinicians and builds institutional trust in AI capabilities. From there, expand into clinical reasoning, safety surveillance, and operational optimization in a phased approach that matches your organization’s readiness and governance maturity.