Healthcare systems worldwide face a growing challenge: rising patient demand, aging populations, and limited human resources. Physician shortages, burnout, and administrative overload threaten care quality, access, and sustainability.
Large Language Models (LLM), Natural language processing (NLP) and workflow automation offer one of the most promising paths to alleviate these pressures. This article explores how AI can help address physician staffing shortages, what it can realistically achieve, where its limits lie, and how domain‑tuned solutions (such as from John Snow Labs) can support safe, effective deployment.
Why physician shortage is a crisis and why it is getting worse
Global and systemic shortage of physicians
- Many countries report shortages of physicians and other healthcare workers. Growing demand (aging populations, chronic diseases, expanded access) exacerbates this gap. According to a recent report, the shortage of healthcare workers remains a critical constraint for many health systems worldwide.*
- The shortage creates cascading burdens: overworked clinicians, long waiting times, and limited access, especially in underserved, rural, or low‑resource settings.
Administrative burden contributes to burnout and inefficiency
- Physicians spend a large portion of their time on documentation, charting, coding, billing, and other administrative tasks rather than direct patient care. This reduces capacity, increases burnout, and makes retention difficult.
- Burnout, work overload, and declining job satisfaction lead to attrition worsening the shortage problem.
Given these pressures, simply hiring more physicians may not be enough. There is a need to rethink workflows, redistribute tasks, and leverage technology to augment clinician capacity rather than replace it.
How AI can ease the burden
AI will unlikely “solve” the shortage alone, but it can significantly optimize how existing clinicians spend their time, increase throughput, reduce waste, and enable task shifting. Here are the main levers:
Automating Clinical Documentation and Administrative Tasks
- AI-powered medical scribes / ambient documentation: Tools that transcribe doctor‑patient conversations or summarize visit notes can drastically reduce the time physicians spend on charting. Ambient documentation systems allow clinicians to focus on the patient rather than typing or dictating notes.
- De‑identification, coding, billing support: NLP can extract structured data from unstructured notes (diagnoses, procedures, prescriptions), map them to standard terminologies (ICD, SNOMED, CPT), and support downstream billing or quality‑measure workflows reducing administrative burden and errors.
- Triage, patient‑message handling, and follow-up automation: AI assistants or chatbots (when appropriately designed and supervised) can draft responses, prepare follow‑up notes, manage appointment scheduling or reminders thus offloading non‑clinical workload from physicians.
By reducing the time spent on paperwork, documentation, and administrative overhead, AI helps free up clinician time for direct patient care, thereby increasing effective capacity without increasing headcount.
Supporting Clinical Decision-Making & Workflow Efficiency
- AI‑assisted diagnostics, triage, risk prediction, and decision support: By analyzing large volumes of patient data (clinical notes, labs, imaging, prior history), AI can help flag high-risk patients, suggest differential diagnoses, recommend follow-up or further tests effectively acting as a “clinical assistant,” helping clinicians see more patients with safety.
- Standardization & consistency: AI reduces variability in documentation, coding, and interpretation which helps reduce errors, improve quality, and speed up workflows. This makes clinician time more efficient and less wasteful.
Optimizing Resource Allocation and Operational Efficiency
- Workforce scheduling & staffing optimization: Some AI tools now support predicting demand, forecasting peaks, optimizing shift schedules, and allocating staff (clinicians, nurses) more efficiently enabling existing workforce to cover more patients with less waste.
- Task‑shifting and role augmentation: By enabling non‑physician staff (nurse practitioners, physician assistants, allied health) to take on more tasks, physician workload can be reduced without compromising care.
Enabling Telehealth, Remote Care, and Access in Underserved Areas
- In regions with physician scarcity (rural areas, low-resource settings), AI‑enabled triage and remote decision support can enable limited physician resources to stretch further.
- By increasing the clinical impact of the physicians time, AI makes sustainable care delivery in challenging environments more feasible.
What AI cannot (yet) do
It is important to acknowledge that while AI helps, it is not a panacea. Several recent analyses caution against over‑reliance on AI to solve workforce shortages entirely.
- AI does not replace clinical judgment: Diagnosis, complex decision‑making, empathy, ethics, and patient communication require human clinicians. AI serves as an assistant, not a substitute. Many professional bodies assert that final decision‑making and communication should remain in human hands.
- Implementation complexity, variability, and risk: AI tools must be validated, integrated into workflows, governed, and monitored. Poor integration or over-trust in AI outputs may introduce errors, quality variation, or risk.
- Not a quick fix for shortage: According to a recent global report, although AI can reduce administrative burden and help efficiency, it “will not be enough to significantly alleviate the shortage of physicians” in many systems.
- Need for supplementary workforce models: AI is most effective when combined with task‑shifting, workforce planning, training, and human‑centered change management.
In summary: AI helps, but only as part of a broader, systemic solution that combines technology, workforce planning, new care models, and human‑AI collaboration.
How John Snow Labs tools can support AI‑driven workforce mitigation
For health systems, payers, clinics, and hospitals considering AI to relieve clinician workload, domain‑tuned infrastructure and reliable pipelines are critical. This is where John Snow Labs can play a pivotal role.
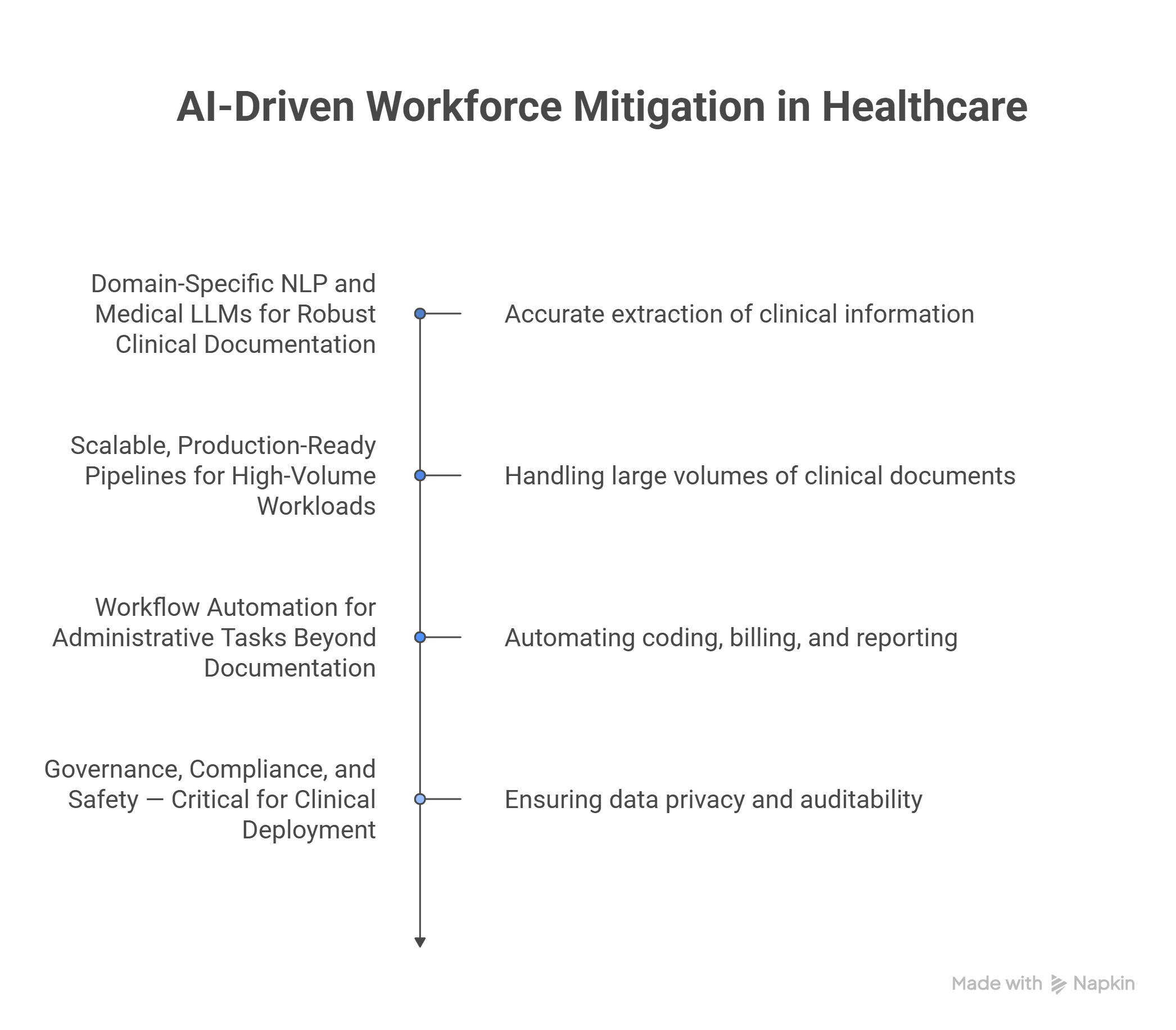
Domain‑Specific NLP and Medical LLMs for Robust Clinical Documentation
- John Snow Labs’sHealthcare NLP and medical LLM models are trained on real-world clinical text (notes, reports, discharge summaries) making them more accurate and reliable than generic models for extracting diagnosis, medications, labs, procedures, and contextual information (temporality, negation, assertion). This reduces the need for manual correction and improves documentation quality.
- Our tools support structured output, coding, normalization enabling converted notes to integrate into EHRs, billing systems, quality‑measure pipelines, and registries. As a result, manual data entry and fragmentation are minimized.
Scalable, Production‑Ready Pipelines for High-Volume Workloads
- Built on scalable big‑data frameworks (Apache Spark), John Snow Labs pipelines can handle large volumes of clinical documents, summary generation, coding, and data extraction enabling institutions to process notes at scale rather than relying on human scribes or manual abstraction.
- This scalability makes it realistic to deploy AI-assisted documentation across entire hospital systems, long-term care facilities, or multi‑clinic networks, thereby offering real impact on clinician capacity and workload.
Workflow Automation for Administrative Tasks Beyond Documentation
- Beyond notes, John Snow Labs tools can support automated extraction for coding, billing, quality‑measure tracking, compliance, and reporting.
- When combined with complementary tools (scheduling, triage, alerting), this creates a comprehensive automation layer that enables clinicians to focus on care while support tasks are handled by AI‑backed pipelines.
Governance, Compliance, and Safety
- Because John Snow Labs allows on‑premises or secure‑cloud deployment, institutions retain full control over patient data. This is essential for privacy compliance, audits, and governance.
- The domain‑tuned nature and traceable outputs support auditability, quality control, and integration with EHR workflows, reducing risk of errors or unmanaged AI behavior.
In short: John Snow Labs’s stack provides the building blocks for AI-assisted clinical capacity but it must be deployed thoughtfully, with human‑in‑the‑loop oversight and strong governance.
What a practical implementation strategy looks like — roadmap for healthcare organizations
Here is a high‑level roadmap for how a hospital / health system / clinic network could deploy AI to help mitigate physician shortage:
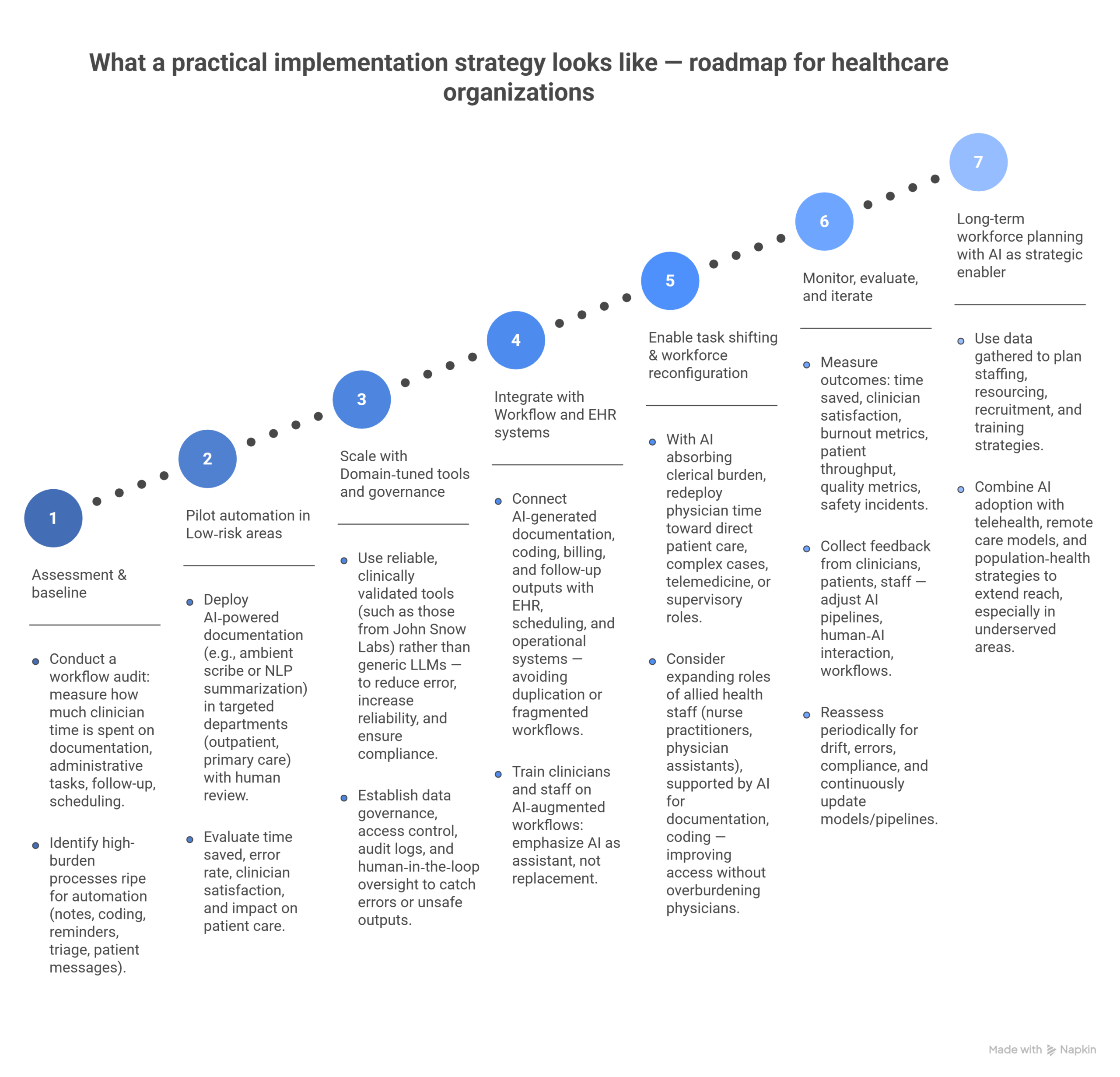
- Assessment & baseline
- Conduct a workflow audit: measure how much clinician time is spent on documentation, administrative tasks, follow-up, scheduling.
- Identify high-burden processes ripe for automation (notes, coding, reminders, triage, patient messages).
- Pilot automation in Low‑risk areas
- Deploy AI‑powered documentation (e.g., ambient scribe or NLP summarization) in targeted departments (outpatient, primary care) with human review.
- Evaluate time saved, error rate, clinician satisfaction, and impact on patient care.
- Scale with Domain‑tuned tools and governance
- Use reliable, clinically validated tools (such as those from John Snow Labs) rather than generic LLMs to reduce error, increase reliability, and ensure compliance.
- Establish data governance, access control, audit logs, and human‑in‑the‑loop oversight to catch errors or unsafe outputs.
- Integrate with Workflow and EHR systems
- Connect AI‑generated documentation, coding, billing, and follow-up outputs with EHR, scheduling, and operational systems avoiding duplication or fragmented workflows.
- Train clinicians and staff on AI‑augmented workflows: emphasize AI as assistant, not replacement.
- Enable task shifting & workforce reconfiguration
- With AI absorbing clerical burden, redeploy physician time toward direct patient care, complex cases, telemedicine, or supervisory roles.
- Consider expanding roles of allied health staff (nurse practitioners, physician assistants), supported by AI for documentation, coding. The goal is to improve access without overburdening physicians.
- Monitor, evaluate, and iterate
- Measure outcomes: time saved, clinician satisfaction, burnout metrics, patient throughput, quality metrics, safety incidents.
- Collect feedback from clinicians, patients, staff. Then adjust AI pipelines, human‑AI interaction, and workflows.
- Reassess periodically for drift, errors, compliance, and continuously update models/pipelines.
- Long-term workforce planning with AI as strategic enabler
- Use data gathered to plan staffing, resourcing, recruitment, and training strategies.
- Combine AI adoption with telehealth, remote care models, and population‑health strategies to extend reach, especially in underserved areas.
What are the realistic potential gains (and limits)
AI in clinical workflows can produce measurable benefits:
- Reductions in documentation time and after-hours charting, helping reduce burnout and improving clinician satisfaction.
- Increased capacity for patient care without proportional increases in staffing by shifting administrative load away from physicians and enabling focus on clinical tasks.
- Improvements in workflow efficiency, consistency, data accuracy, and standardization (documentation, coding, follow‑up).
- Better coverage of underserved populations via remote care, task shifting, and more efficient use of limited physician time.
Yet AI will not by itself solve physician shortage. According to a recent international analysis, while AI can reduce clinician burden and support expanded productivity, it does not replace the need for human clinicians.*
The realistic expectation is that AI becomes an amplifier of human clinical capacity, enabling existing clinicians to deliver more, reducing burnout, and improving sustainability especially when combined with restructured care, task‑shifting, and system-level workforce planning.
Conclusion: toward augmented healthcare capacity, not replacement
The physician shortage crisis is real, widespread, and complex. It is driven by demographic changes, growing demand, attrition, inefficiencies, and expanding care needs. While AI cannot “grow” the number of doctors overnight, it offers a powerful lever to optimize how existing clinicians work, reduce waste, free time, and enable more with less.
Used thoughtfully, with domain‑tuned tools, robust governance, integration into workflows, and human‑in‑the‑loop oversight, AI can become a strategic ally, helping address population health demands, relieve clinician burnout, and improve access. Providers, health systems, and policymakers should treat AI not as a magic bullet, but as a force multiplier: a way to stretch scarce resources responsibly, expand capacity, and build a more sustainable, human‑centered healthcare system.